This is the most comprehensive medical resource for trekking the Rwenzori Mountains, covering altitude illness, hypothermia, infections, field medicine, and evacuation risks.
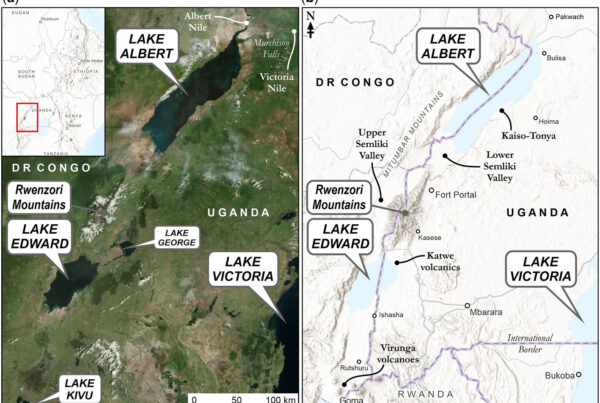
The Rwenzori Mountains of Uganda and the Democratic Republic of Congo, often called the “Mountains of the Moon,” are among the most medically complex trekking environments on Earth. Unlike arid alpine ranges, the Rwenzori combine equatorial altitude, persistent cold rain, glaciation, high humidity, swamps, remote access, and limited evacuation infrastructure into a uniquely hostile physiological setting.
Trekkers face simultaneous stressors rarely encountered together: hypobaric hypoxia (low oxygen pressure) at altitude, thermal stress from wet cold, high infection exposure, rapid weather shifts, and logistical isolation. These interact to increase the risk of acute mountain sickness (AMS), hypothermia, respiratory infections, foot immersion injuries, wound infections, dehydration, and decision-making impairment.
This guide synthesizes high-trust principles from wilderness medicine, high-altitude physiology, expedition planning, and tropical medicine to provide the most technically rigorous medical framework currently available for Rwenzori trekking. It assumes readers already understand basic trekking practices and focuses instead on failure modes, evidence-based risk reduction strategies, and operational medical planning.
This is not medical advice for individuals. It is a field-level technical reference designed to support informed decision-making by trekkers, guides, researchers, journalists, and expedition planners.

Mount Stanely Glacier
Overview of the Rwenzori Medical Environment
The Rwenzori Mountains rise abruptly from equatorial lowlands to glaciated peaks exceeding 5,000 meters (Mount Stanley 5,109 m / 16,763 ft). Unlike most high world mountains, they sit almost exactly on the equator, producing:
-
High precipitation year-round (often >2,000 mm rain annually)
-
Persistent cloud cover
-
Cold temperatures at altitude combined with wet exposure
-
Boggy alpine zones
-
Rapid daily weather shifts
Rwenzori Treks typically last 6–12 days and involve prolonged exposure to cold rain, steep terrain, deep mud, river crossings, and limited shelter.
Medical infrastructure within the Rwenzori range is extremely limited No hospitals inside park boundaries, Minimal helicopter rescue availability since most of the rescue is made by Porters and Most evacuations involve porter carry-outs over multi-day terrain to the near by hospital in Kasese.

Huts in the Rwenzori Mountain
As a result Medical self-sufficiency is mandatory, early recognition and conservative decision-making are critical before the hike and delays worsen outcomes for altitude illness, hypothermia, sepsis, and trauma. So every after the hiking day our professional guides have to ask you if still can continue up or your health is detoriating so they can give you porters to carry you back or if you still have energy you can trek down the Mountain while being monitered.
How the Body Responds to the Rwenzori Environment
When ascending to high altitude, the most crtical change is reduced oxygen availability in higher regions of the mountain. Even though the air still contains the same percentage of oxygen, the pressure is lower, so less oxygen enters the bloodstream with each breath. The body responds by breathing faster and deeper, increasing heart rate, and gradually making changes that improve oxygen delivery to tissues. This adaptation process is called acclimatization. It takes time. Moving too fast overwhelms it.
At the same time, cold and wet exposure increase energy demands. The body burns more calories to stay warm. Appetite often decreases at altitude, and digestion slows. This combination leads to energy deficits that worsen fatigue, impair immune function, and slow recovery from injury.
Cold exposure causes blood vessels in the skin and extremities to constrict, reducing heat loss but also reducing sensation and dexterity. Prolonged wet exposure softens the skin and damages its protective barrier, increasing the risk of blisters, fungal infections, and bacterial skin infections.
Sleep quality deteriorates at altitude due to breathing instability and cold discomfort. Poor sleep worsens mood, judgment, coordination, and reaction time. These effects increase the risk of accidents and reduce tolerance to stress.
Finally, immune function becomes less efficient under the combined effects of cold stress, dehydration, calorie deficit, and altitude exposure. This increases susceptibility to respiratory infections, skin infections, and gastrointestinal illness.
None of these changes are dangerous on their own. Together, over multiple days, they can create a medical situation where small problems escalate quickly unless recognized early and managed conservatively.
Altitude Illness in the Rwenzori
Altitude sickness is the most serious and potentially fatal medical risk on Rwenzori and other high-altitude treks. It occurs when the body fails to adapt adequately to reduced oxygen levels after ascent. It does not require extreme altitude and can occur below 3,000 meters in susceptible individuals, though risk increases with elevation and rate of ascent.
There are three main forms of altitude illness. The mildest and most common is acute mountain sickness, often abbreviated AMS. More severe and life-threatening forms of altitude illness include high-altitude cerebral edema, which affects the brain, and high-altitude pulmonary edema, which affects the lungs; however, these conditions are rare in the Rwenzori Mountains and mostly occur at very high altitudes, such as those found on Mount Everest.

Acute mountain sickness usually begins with a headache and is often accompanied by nausea, fatigue, dizziness, loss of appetite, and disturbed sleep. These symptoms typically appear within several hours to one day after ascent. Mild AMS can resolve with rest and time at the same altitude. However, worsening symptoms or progression to neurological or respiratory symptoms indicates more serious disease.
High-altitude cerebral edema involves swelling brain tissue. Early signs include difficulty walking in a straight line, clumsiness, confusion, unusual behavior, severe fatigue, and worsening headache. This condition can progress rapidly to coma and death if descent is delayed.
High-altitude pulmonary edema involves fluid accumulation in the lungs. Early signs include shortness of breath with exertion that seems worse than expected, reduced exercise tolerance, and persistent cough. Later signs include shortness of breath at rest, chest tightness, bluish lips or fingernails, and coughing up frothy or pink sputum. This condition is often fatal without prompt descent.
Altitude illness does not correlate with fitness, strength, or experience. Highly trained athletes develop it just as frequently as untrained individuals. Although prior altitude illness heightens future risk, it can affect anyone.
The most important risk factor is rapid ascent. Many Rwenzori itineraries climb quickly from low elevations to sleeping camps above 3,500 or 4,000 meters within two or three days. This pace exceeds conservative acclimatization recommendations and increases illness risk substantially.
Other risk factors include dehydration, respiratory infection, excessive exertion early in ascent, poor sleep, alcohol use, and prior history of altitude illness. Diagnosis in the field is clinical. There is no blood test or device that can reliably rule out altitude illness. Pulse oximeters may show low oxygen saturation, but values vary widely among healthy people at altitude and cannot be used alone to make decisions. Symptoms and functional changes matter more than numbers.
Prevention focuses on slow ascent, rest days, hydration, nutrition, and avoidance of alcohol and sedatives. Some trekkers use acetazolamide, a medication that stimulates breathing and improves oxygenation. This method reduces the risk and severity of AMS but does not eliminate it. It must be started before ascent and continued during altitude exposure. It is not a substitute for conservative assent.
Treatment of mild AMS involves stopping ascent, resting at the same altitude, maintaining hydration, using pain relievers for headache, and possibly starting acetazolamide if not already taking it. If symptoms improve, ascent can resume cautiously. Descent is necessary if symptoms get worse or don’t get better after resting.
Treatment of high-altitude cerebral edema or pulmonary edema requires immediate descent. Oxygen and medications such as dexamethasone for cerebral edema or nifedipine for pulmonary edema can stabilize patients temporarily, but they do not cure the condition. Descent is the only definitive treatment. Delayed descent is the main cause of fatal outcomes in altitude illness worldwide.
One of the most dangerous mistakes in mountain medicine is continuing to climb while symptomatic, especially when symptoms are masked with painkillers or stimulants. Another common failure mode is waiting overnight to see if symptoms improve. In the Rwenzori, where weather can worsen suddenly and evacuation is slow, early descent saves lives.
Cold Exposure and Hypothermia
Hypothermia, defined as a core body temperature below 35°C (95°F), is a major medical risk in the Rwenzori. Unlike high-altitude deserts or dry alpine environments, the Rwenzori expose trekkers to constant rain, wet vegetation, river crossings, fog, and wind. Even when air temperatures are only mildly cold, wet clothing and wind dramatically accelerate heat loss. Hypothermia can develop at temperatures well above freezing.

Early hypothermia usually presents with shivering, cold discomfort, clumsiness, fatigue, and impaired fine motor skills. As it worsens, shivering may become violent or stop entirely, speech becomes slurred, thinking becomes confused, coordination deteriorates, and heart rhythm disturbances may occur. Severe hypothermia can cause unconsciousness and death.
Hypothermia is dangerous because it impairs judgment and coordination. Hypothermic trekkers make poor decisions, stumble more easily, and are less able to perform basic tasks such as changing clothes, setting up shelter, or preparing food. Such behavior creates a downward spiral.
Preventing hypothermia relies on using layered clothing systems that retain insulation when wet, having reliable waterproof shells, making frequent clothing changes, maintaining a high-calorie intake, and minimizing prolonged exposure during rest breaks. Synthetic insulation is often more reliable than down in persistently wet environments. Hands, feet, and head require special attention.

Preventing hypothermia relies on using layered clothing systems like these
Once hypothermia begins, treatment involves removing wet clothing, insulating the person from the ground, adding dry layers, blocking wind, and providing warm sweet drinks if the person is conscious and able to swallow. Active movement may help in mild cases. Moderate or severe hypothermia requires evacuation and careful rewarming. Rapid aggressive rewarming of extremities alone should be avoided in severe cases, as it can worsen heart rhythm disturbances.
True frostbite is less common in the Rwenzori than in colder or drier alpine environments, but cold-induced numbness, circulation impairment, and tissue injury can occur during summit attempts, especially in windy conditions at high altitude. Gloves, mittens, face protection, and moisture control are critical during these phases.
Infectious Disease Risks
The Rwenzori lie within a tropical ecosystem with high microbial diversity. Combined with immune suppression from altitude, cold exposure, fatigue, and calorie deficit, this increases susceptibility to infection. The most common problems involve the respiratory tract, gastrointestinal system, and skin.
Respiratory infections are frequent. Cold air, high ventilation rates, and airway irritation cause cough and throat discomfort even without infection. However, fever, chest pain, productive cough, and systemic illness suggest infection rather than altitude-related irritation. Respiratory infections worsen oxygenation and can trigger or exacerbate altitude illness.
Gastrointestinal illness is common during travel in many regions of the world and may result from contaminated food, water, or poor hand hygiene. Diarrhea and vomiting lead to dehydration, electrolyte imbalance, weakness, and impaired acclimatization. Severe dehydration increases the risk of altitude illness and hypothermia and reduces physical performance.
Skin and soft tissue infections are particularly common in the Rwenzori due to constant wet exposure, mud, abrasions, insect bites, and delayed wound care. Skin becomes macerated, its protective barrier breaks down, and bacteria enter easily. Minor blisters or cuts can progress to cellulitis or abscesses if not treated promptly.
Vector-borne diseases such as malaria are primarily a concern in lower-elevation approach zones rather than at higher camps, but exposure varies by season and region. Risk assessment and prophylaxis should follow current public health guidance.
Prevention of infection depends on vaccination according to international travel recommendations, consistent hand hygiene, safe water treatment, careful food handling, prompt wound cleaning, and keeping skin as dry as possible in wet conditions. These measures reduce risk but do not eliminate it.
Field management of infection includes early detection, rest, hydration, wound care, and, when necessary, antibiotic treatment with the help of a doctor. Because evacuation is slow, infections that worsen rapidly or involve systemic symptoms require conservative management and early descent.
Pre-Expedition Medical Screening and Preparation
Anyone planning to trek the Rwenzori should undergo basic medical screening, especially if they have a history of heart disease, lung disease, diabetes, neurological disorders, blood clotting disorders, or previous severe altitude illness in other mountains. These conditions do not necessarily prohibit trekking, but they require specialist evaluation and risk assessment while trekking the Rwenzori mountains since they are very remote.
Fitness preparation should focus on aerobic endurance, leg strength, balance, and load carrying. However, fitness does not protect against altitude illness and should not be used as justification for rapid ascent.
Vaccination should follow national and international travel medicine recommendations for East African countries. Commonly recommended vaccines include yellow fever, hepatitis A and B, typhoid, tetanus, and influenza. Requirements vary by country and traveler origin.

Malaria prophylaxis decisions should follow public health guidance based on regional risk. While malaria transmission is minimal at high altitudes, exposure to mosquitoes may occur during travel to and from trekking regions.
Some trekkers use pre-acclimatization strategies such as staged altitude exposure or hypoxic tents. Evidence suggests these may reduce AMS risk in some individuals, but they do not eliminate the need for conservative ascent profiles and symptom monitoring.
Medication planning should include personal prescriptions plus contingency supplies in case of delays, losses, or damage. Trekkers with asthma, diabetes, severe allergies, or other chronic conditions must carry sufficient medication and emergency supplies, including backup devices where applicable.
Medications and Medical Supplies for Rwenzori Treks
Field medical supplies should be designed for wet environments, delayed evacuation, and high-altitude conditions. They must be waterproofed, organized, and accessible. All users should understand indications, dosing, side effects, and contraindications.
Medications that are often taken on Rwenzori treks include pain relievers like ibuprofen and acetaminophen; medications for altitude sickness such as acetazolamide, dexamethasone, and nifedipine; gastrointestinal treatments like oral rehydration salts, anti-nausea drugs, and anti-diarrheal medications; antibiotics for skin, respiratory, or gastrointestinal infections when needed; antihistamines and epinephrine for allergic
Acetazolamide is used to reduce the risk and severity of acute mountain sickness. It works by stimulating breathing and improving oxygenation. Common side effects include tingling sensations in the fingers and toes, increased urination, and altered taste of carbonated beverages. It should be started before ascent and continued during altitude exposure. It does not prevent severe altitude illness and does not replace conservative ascent.
Dexamethasone is used to treat moderate to severe altitude illness affecting the brain. It reduces brain swelling but does not improve acclimatization. It should only be used in conjunction with descent.
Nifedipine is used to treat high-altitude pulmonary edema by lowering pulmonary artery pressure. It does not replace descent.
Antibiotics should be selected under medical supervision, based on likely pathogens, resistance patterns, and individual allergies. Inappropriate use increases adverse effects and antibiotic resistance.
All medications should be stored in waterproof containers and protected from extreme cold, moisture, and physical damage. Expiration dates should be checked before departure.
Oxygen systems and portable hyperbaric chambers may be available on some expeditions. While they can temporarily stabilize patients during delayed descent, they cannot cure altitude illness. They require training, monitoring, and logistical support and should not be relied upon as substitutes for conservative ascent and evacuation planning.
First Aid and Medical Care in the Field
Environment, equipment, personnel, and evacuation constraints limit medical care in the Rwenzori. Field care focuses on early recognition, stabilization, symptom management, and timely descent or evacuation.
Minor problems such as blisters, mild respiratory infections, minor gastrointestinal upset, and musculoskeletal pain should be addressed early before they worsen. Early rest, hydration, wound care, and load adjustment prevent many evacuations.
Serious problems such as worsening altitude illness, hypothermia, significant trauma, severe infection, dehydration with inability to tolerate fluids, or altered mental status require immediate descent and evacuation planning.
Documentation of symptoms, timing, treatments, and response to interventions improves decision-making and handover during evacuation. Clear communication among guides, trekkers, and support staff is essential.
Group management matters. When one person becomes ill, others may need to modify plans, share loads, or assist with evacuation. Expedition leaders must balance individual care with group safety and resource constraints.
Evacuation and Rescue in the Rwenzori
Evacuation from the Rwenzori is slow and physically demanding. Most evacuations involve porter carry-outs over steep, muddy trails. Stretcher evacuation may take many hours or days depending on location, weather, terrain, and personnel availability. Helicopter rescue is rare and unreliable due to weather, terrain, cost, and logistical constraints.
This reality has several implications. First, medical problems must be recognized and treated early. Second, conditions that deteriorate rapidly, such as severe altitude illness, hypothermia, major trauma, and sepsis, must be addressed aggressively before evacuation. Third, expedition planning must assume self-sufficiency for prolonged periods.
Insurance that covers evacuation and rescue is essential but does not guarantee rapid extraction. Contingency planning should include communication systems, evacuation routes, porter availability, and realistic time estimates.
Special Populations and Risk Groups
People with heart disease, lung disease, blood disorders, neurological conditions, diabetes, or immune suppression face increased risks at altitude and in cold, wet environments. These individuals should undergo a specialist evaluation before trekking to ensure their conditions are stable and well-controlled. They must carry adequate medication supplies and contingency plans.
People with asthma or reactive airway disease may experience bronchospasm triggered by cold air and exertion. Inhalers and action plans are essential.
People with diabetes face challenges due to altered appetite, increased energy expenditure, cold effects on glucose monitoring devices, and increased risk of hypoglycemia during prolonged exertion. Careful monitoring and conservative management are required.
Older trekkers are not inherently at higher risk of altitude illness, but comorbidities and reduced physiologic reserve increase vulnerability to complications. Conservative ascent profiles and close monitoring are recommended.
People with prior altitude illness are at higher risk of recurrence and should use prophylactic strategies and conservative itineraries.
Pregnancy, recent surgery, and acute illness require individualized medical evaluation before high-altitude trekking.
Ethical Responsibilities in Guided Expeditions
Guides and expedition leaders carry a duty of care to prioritize safety over objectives. This includes enforcing conservative ascent profiles, monitoring clients with their subtle symptoms, ensuring adequate hydration and nutrition, managing pacing, and making difficult decisions to descend when necessary. Guides must resist social or summit pressure when it compromises safety.
Clients also bear responsibilities. They must disclose relevant medical history honestly, comply with safety decisions, report symptoms early, and avoid self-medicating in ways that mask dangerous conditions.
Informed consent requires that trekkers understand the limits of medical care and rescue in the Rwenzori and accept that outcomes depend heavily on early recognition and conservative decision-making.
Frequently Asked Questions (FAQs) about Medical Procedures in the Rwenzori Mountains.
Is altitude sickness more dangerous in the Rwenzori than on other mountains?
Altitude illness itself is not inherently more dangerous in the Rwenzori than in other ranges, but the environment increases overall risk. Cold rain, fatigue, infection exposure, and delayed evacuation worsen outcomes when altitude illness occurs. Rapid ascent profiles on some itineraries further increase risk.
Does acetazolamide guarantee I will not get altitude sickness?
No. Acetazolamide reduces the risk and severity of acute mountain sickness but does not eliminate it. Severe illness can still occur. Conservative ascent and symptom-based decision-making remain essential.
Does physical fitness protect against altitude illness?
No. Fitness improves endurance and reduces injury risk but does not reduce susceptibility to altitude illness. Highly trained athletes develop AMS, HACE, and HAPE at the same rates as less fit individuals.
How cold does it get in the Rwenzori?
Temperatures near the summits often drop below freezing, especially at night and in wind. More importantly, persistent rain and wet exposure at lower temperatures significantly increase hypothermia risk even when air temperatures are above freezing.
Is malaria a risk during Rwenzori treks?
Malaria risk exists primarily at lower elevations and during travel to and from trekking areas. Transmission at high camps is minimal. Risk assessment and prophylaxis should follow current public health guidance.
What is the most common medical reason for evacuation?
Altitude illness is the most common serious medical reason for evacuation, followed by musculoskeletal injuries and infections.
Can oxygen prevent descent in altitude illness?
Oxygen may temporarily improve symptoms but does not reverse acclimatization failure. Descent remains the only definitive treatment for serious altitude illness.
How long does evacuation usually take?
Evacuation may take anywhere from 12 hours to several days depending on location, weather, terrain, and resources. Rapid evacuation cannot be assumed.
Are antibiotics necessary for most infections on the trail?
No. Many infections resolve with rest, hydration, and local care. Antibiotics should be reserved for clinically significant infections under appropriate guidance.
Can sleeping pills be used safely at altitude?
Sedatives and alcohol depress breathing and worsen hypoxia and should be avoided. Acetazolamide may improve sleep by stabilizing breathing patterns.
What single decision saves the most lives in the mountains?
When serious symptoms appear, it is crucial to make an early descent. Delayed descent is the most common cause of fatal outcomes in altitude illness worldwide.